CareGuard is Ametros' professional administration service. With CareGuard, the Company sets up a bank account for the injured party's settlement funds and acts as the custodian of the funds and the third party administrator paying for all healthcare expenses. The CareGuard service manages everything for the injured party, including the coordination and payment of medical bills as well as any necessary reporting to Medicare. This differs from Ametros' self-administration service Amethyst, because the funds are put into a custodial account that is fully managed on behalf of the injured party.
CareGuard
What happens after I settle my case with Ametros’ CareGuard service?
Our Care Advocate team will reach out to begin the onboarding process. We will setup your account, explain how it works, and gather your doctor and pharmacy information. We reach out to your doctors and pharmacies to make sure they know you will be using CareGuard from now on and that they can bill CareGuard directly. A welcome package including your CareGuard card will be sent to you in the mail. Once you receive the card, you can take it to your doctor or pharmacy and you will not have a copay; all the bills will be directed to CareGuard. CareGuard will review them for accuracy, apply discounts to reduce them, if applicable, and then pay from your account on your behalf. If you have a Medicare Set Aside, CareGuard will file all your reporting to Medicare for you to make sure you are in compliance and that your benefits are protected.
Who notifies my doctors/how do they find out about CareGuard?
When you become a CareGuard member, our team will find out all the doctors, providers and pharmacies you are seeing. We then will contact them to provide them with information on how to bill CareGuard for all future expenses. We also provide you with information explaining CareGuard in your welcome packet in case you go to a new provider and our team has not been notified to call ahead.
Who has access to my CareGuard account?
Unless you designate someone, only you and CareGuard representatives have access to your account. Representatives have access in order to help you compile your reporting or assist you through our Care Advocate Team. We take your identity and information security very seriously and have rigorous security protocols to protect your account.
How do I use my CareGuard card?
The CareGuard card acts like a traditional insurance card. When you go to the doctor or pharmacy, simply show your CareGuard card at check in, and bills will automatically be sent to our Care Advocate team. There are no co-pays with the CareGuard card, and, once we receive the bill we will provide any network savings, and then pay on your behalf.
Is the CareGuard Card a debit card?
The CareGuard card functions like traditional insurance card and cannot be used like a debit card. The CareGuard card can only be used to notify doctors and pharmacies to send bill directly to CareGuard. You cannot withdraw money from your CareGuard account on demand. The account contains your medical funds from your settlement and is established in accordance with the terms of your settlement agreement. To learn more about deposits or withdrawals from your CareGuard account contact our Care Advocate team.
Can I withdraw funds from my CareGuard account?
You cannot withdraw money from your CareGuard account on demand. The account contains your medical funds from your settlement and is established in accordance with the terms of your settlement agreement. In some situations, you can withdraw funds and, in others, it is not permitted. To learn more about possible deposits or withdrawals from your CareGuard account contact our Care Advocate team.
What happens if I run out of money?
Should your funds exhaust, we will notify you and Medicare that the account has exhausted. Your providers should still bill CareGuard for your treatment. They will receive communication in the form of an Explanation of Benefits (EOB) with a denial instructing them to bill your secondary insurance if the fund has exhausted. At this point, you will need to provide your secondary insurance information to your provider if you have not already done so. CareGuard is unable to reimburse for copays or deductibles per CMS guidelines. If you have an annuity, once your funds are replenished, your MSA account will then be used to reimburse your providers as the primary payor.
What if I need a new doctor?
With CareGuard, you can see any doctor you would like, with no restrictions. If you need to switch doctors/pharmacies, we ask that you please give us a call. We will reach out to them and make sure CareGuard is setup in their system as the payor for your medical bills. That way, when you show up for your visit, you only have to mention CareGuard and everything will be ready to go. Please note, you can choose any doctor/pharmacy you want; they do not have to be within our network. Our Care Advocate team will help you find doctors or pharmacies. Just give us a call!
What if I need to change medications?
As time goes on, medication and treatment will change. Just give us a call at 877.275.7415 and we will update our records with the new information. If you have a Medicare Set Aside, we will help advise you on what medications are eligible for payment by your MSA.
What happens if Ametros goes out of business?
Your CareGuard account is set up under your name and Social Security number or Tax Identification Number. Each account is a separate bank account with FDIC insurance. The funds in your account are never a business asset of Ametros. This ensures your account will be always protected should Ametros ever become insolvent in the future.
What do I do if I have any out-of-pocket expenses?
Any covered out-of-pocket expenses related to your injury can be reimbursed upon submission of a receipt. You can submit receipts for reimbursement through your CareGuard member portal or fax or mail them in for review.
Who can I contact for more help?
Ametros is staffed with a fantastic Care Advocate Team that are available to you 24/7, by email, phone or online chat. They are there to be your support system for questions, concerns, and to help coordinate your care.
What happens if I pass away?
Frequently in workers compensation and liability settlements there is a provision in the settlement agreement that governs the person(s) or entity(ies) (the “beneficiary(ies)”) that will receive what remains of the medical settlement funds in an administered account upon the death of the injured person. The parties to the settlement on both the plaintiff and defense side may negotiate this provision and place certain stipulations on how the remaining funds are disbursed. Upon death of the account holder, Ametros reviews these terms in the settlement agreement and disburses funds to the beneficiary(ies) that are named. If there is no beneficiary named, the funds will pass on to the account holder’s estate or according to their will. If there is no beneficiary(ies) named in the settlement agreement, nor an estate plan or will, the member can fill out a beneficiary form with Ametros. For clarity, any instructions in the executed settlement agreement always take priority in governing the disbursement. Regardless of the beneficiary(ies), Ametros does not charge an account closing fee or retain any of the remaining funds in the account.
Do I have to see a specific doctor?
You are able to treat with any doctor/pharmacy you’d like; they do not have to be a part of our network for you to use CareGuard and potentially receive our discounts on healthcare expenses. While not required, many members choose to use CareGuard’s network providers so that they can save more on every visit.
Does Ametros dictate my treatment?
With your CareGuard membership, you are free from utilization review. In most instances of a Medicare Set Aside (MSA), so long as your treatment is related to your underlying claim and otherwise covered by Medicare, the expenses will be covered. In other instances, it’s possible there are no limitations with respect to the scope of your covered treatment. Your treatment plan is typically at the discretion of you and your doctor.
What happens if I don’t use all my funds in a given year?
Each year your remaining funds will remain in the account and roll into the next year.
Does the carrier or employer have any input into any of my treatment?
After settling out your case, the carrier or employer does not have any input on your ongoing treatments.
What happens if my bills exceed the amount in my account?
If the yearly funds run out, Ametros will help coordinate with any secondary form of insurance or payment you may have, including Medicare coverage. Typically, a member’s secondary insurance will step in and pay for the remaining balance of your bills. For members with a Medicare Set Aside (MSA), that secondary insurance is Medicare coverage. When you use secondary insurance, including Medicare, you will still be responsible for any deductibles and copays personally or through the secondary insurance. If you have an MSA and an annuity, once your account is replenished, CareGuard will become the primary payer again with your MSA funds.
Will Ametros negotiate the treatment or service prices with providers?
We run bills through our network and reprice to the appropriate fee schedule or network discount. If the provider is within our network, we are often able to provide additional savings below the fee schedule or typical “usual and customary” price. Through Ametros’ discount networks you may potentially save an estimated 62% on provider visits and an estimated 28% on your prescriptions. Our team reviews every bill for possible savings, in efforts to make your funds last longer.*
For large bills and with providers that are out of network, CareGuard’s team will still attempt to negotiate discounts
Does Ametros have the authority to determine medical necessity?
No. Medical necessity is to be determined by a licensed medical professional. Ametros does not direct care nor determine necessity.
Are members taxed on interest that the CareGuard account earns?
CareGuard establishes a bank account for the member that earns interest. Just like with any other bank account, the federal government taxes interest earned. The member will receive a 1099-INT if the account earns more than $10.00 in interest. For members with a Medicare Set Aside, according to Medicare’s guidelines, the funds in the MSA account can be used to pay for taxes on the interest earned by the account.
How do I sign up for the CareGuard Member Portal?
How do I sign up for the CareGuard Member Portal?
As a CareGuard member, you always have full visibility into your account activity and savings with your CareGuard Member Portal.
Set Up Your Online Account in 5 Simple Steps
- Go to https://portal.careguard.com/#/login.
- Click 'Register'
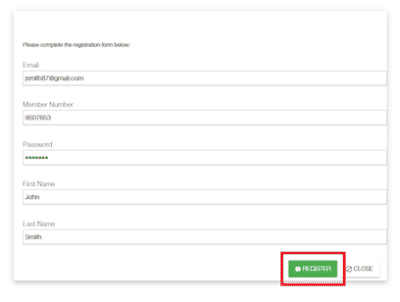
- Complete the registration form by filling out your name, email, membership ID #, and then choose a password
- Please reference you membership ID# on the back of your CareGuard card during registration
- Click ‘Register’ on the registration form
- Please finish setting up your account by clicking the validation link sent to your email